In the future, viable piglets, with blood vessels that will be an exact match to the patient, could ensure a successful transplant.
March 17, 2020
A team of researchers at the University of Minnesota Medical School recently proved the ability to grow human-derived blood vessels in a pig—a novel approach that has the potential for providing unlimited human vessels for transplant purposes. Because these vessels were made with patient-derived skin cells, researchers say they are less likely to be rejected by the recipient, helping patients potentially avoid the need for life-long, anti-rejection drugs.
Daniel Garry, MD, PhD, and Mary Garry, PhD, both professors in the Department of Medicine at the UMN Medical School, co-led the research team and published their findings in Nature Biotechnology last week.
"There's so many chronic and terminal diseases, and many people are not able to participate in organ transplantation," says Daniel, who is also a heart failure and transplant cardiologist. "About 98% of people are not going to be eligible for a heart transplant, so there's been a huge effort in trying to come up with strategies to increase the donor pool. Our approach looked at a pig."
Because of similarities between human and pig physiology, scientists have historically studied pigs to discover treatments for health issues, including diabetes. Before researchers engineered human insulin, doctors treated patients with pig insulin.
"Our discovery has made a platform for making human blood vessels in a pig," says Daniel. "This could allow us to make organs with human blood vessels that would be less apt to be rejected and could be used in patients in need of a transplant. That's what typically causes rejection—the lining of the blood vessels in the organs."
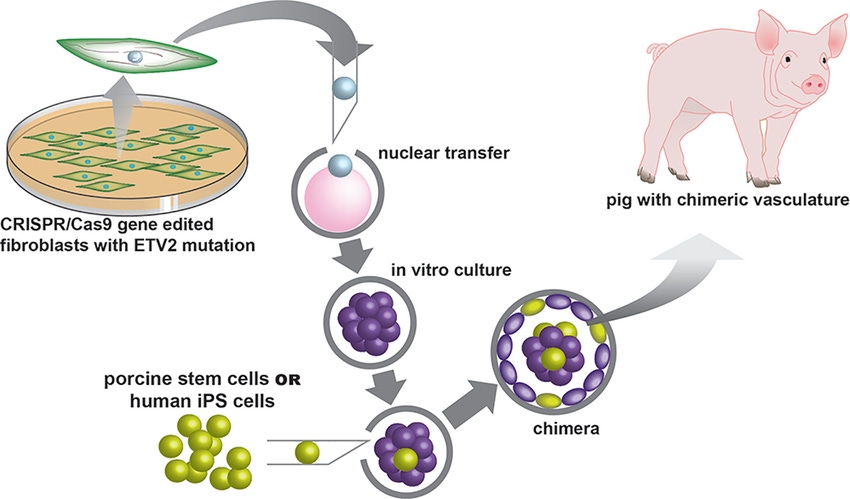
The blood vessels created by the Garry duo will avoid rejection because of the method by which they are made. The team injects human-induced pluripotent stem cells—taken from mature cells scraped from a patient's skin and reprogrammed to a stem cell state—into a pig embryo, which is then placed into a surrogate pig. In the future, viable piglets, with blood vessels that will be an exact match to the patient, will ensure a successful transplant and the ability to live without the need for immunosuppression, or anti-rejection, drugs.
"There's hundreds of thousands of patients that have peripheral artery disease, either because of smoking or diabetes or any number of causes, and they have limb amputations," Mary says. "These blood vessels would be engineered and could be utilized in these patients to prevent those kinds of life-long handicaps, if you will."
The first phase of their study, approved by the UMN Stem Cell Research Oversight committee, brought the first embryo to a 27-day term. Because of the success of this phase, Daniel and Mary are currently seeking the committee's approval to advance the research further into the later gestational period.
"We're trying to take it in a phased approach," Daniel says. "We want to be sure we address all of the possible issues—whether human cells go where we want them to go."
"While it is a first phase, there's pretty solid proof of concept," Mary says. "We believe that we've proven that there's no off-target effects of these cells, so we're ready to move forward to later gestational stages."
Current UMN investigators who participated in this study include Satya Das, Naoko Koyano-Nakagawa, Geunho Maeng, Bhairab Singh, Daniel Mickelson, Wuming Gong, Cyprian Weaver, Stefan Kren and Demetris Yannopoulos.
Source: University of Minnesota Medical School, which is solely responsible for the information provided, and wholly owns the information. Informa Business Media and all its subsidiaries are not responsible for any of the content contained in this information asset.
You May Also Like



