Pig Health Impacts Carcass Contamination, Food Safety
An Iowa State University study quantitatively demonstrates the link between food animal production practices and human health implications for food safety.
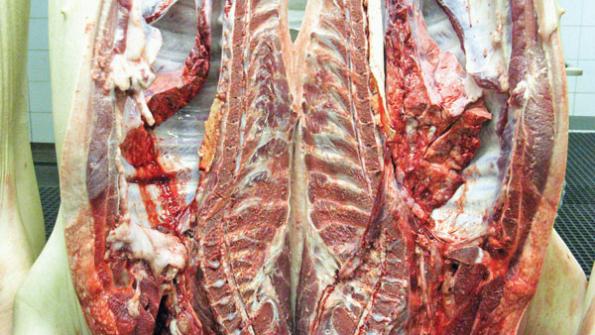
Close inspection prior to slaughter will definitely preclude pigs with clinical signs of disease from being harvested. But subclinically ill pigs, those that show no visible signs of being sick, can pass inspection and thereby pose a public health hazard. Of particular concern is the potential increase in carcass contamination with salmonella and campylobacter, because those bacteria can also be shed and spread by animals at the packing plant.
Few studies have quantitatively demonstrated the link between food animal production practices and human health implications for food safety.
One study, using pooled samples of swine carcasses with tissue damage or lesions indicative of chronic infection, showed for every 1% increase in peelouts, there was a 5% increase in contamination with enterococcus and campylobacter bacteria at the end of processing compared with carcasses without lesions. However, researchers failed to establish a definite link between peelouts (removal of the pleural and peritoneal linings after evisceration) and salmonella contamination.
New Approach
Scott Hurd, DVM, associate professor of the Veterinary Diagnostic and Production Animal Medicine Department in the College of Veterinary Medicine at Iowa State University, led a study to determine the link between lesions suggestive of subclinical illness in pigs and salmonella carcass contamination through testing of individually swabbed carcasses.
In the study, pigs representing two types of production practices were selected — antibiotic-free and conventionally raised. To avoid the potential confounder of barn of origin, sample pigs originated from one barn and were managed with the same veterinary care, housing, environment and feed. Pigs were evaluated on two separate days in a large midwestern packing plant, Hurd points out.
The carcasses were evaluated for lesions by a third-year veterinary student trained by a veterinary pathologist. Photos were taken of all carcasses and scored by three veterinary pathologists.
Results
The study included 358 carcasses from 156 pigs raised without antibiotics and 202 pigs raised conventionally and administered antimicrobials for disease prevention and treatment.
Salmonella was recovered from 36 of 358 carcasses (10.1%). Enterococcus was recovered from 39 of 358 carcasses (10.9%). The prevalence of carcasses with salmonella differed greatly across the four replicates of the study, with prevalence in the first trial (1%) much lower than later trials (up to 10%).
“Carcasses of swine raised without antimicrobials were significantly more likely to be contaminated with salmonella (27 of 156; 17.3%) than carcasses of conventionally raised pigs (9 o f 202; 4.5%),” Hurd says. Carcasses of conventionally raised swine had a slightly higher probability of enterococcus contamination.
There was close agreement among swine veterinary pathologists on lesion scores, and there was very close agreement between the evaluations of the pathologists and the scores of the non-expert veterinary students.
The non-expert evaluators identified 182 carcasses as having lesions. Of these, 22 (12%) had positive results for salmonella and 22 (12%) had positive results for enterococcus.
In contrast, 8% and 10% of the carcasses judged as not having lesions had salmonella and enterococcus contamination, respectively.
Further analysis of the association between bacterial contamination and lesion status as defined by non-expert assessment revealed that carcasses judged as having lesions were 90% more likely to have salmonella contamination than carcasses without lesions, he says.
There was no difference in probability of enterococcus contamination regardless of carcass lesions.
The design of this study did not provide a reason for increased likelihood of pathogen contamination of carcasses with lesions vs. carcasses without lesions nor accurately compare antibiotic-free and conventionally raised swine production methods.
Carcasses of antibiotic-free pigs had a much higher probability of salmonella contamination than did carcasses from conventionally raised pigs.
“The use of carcass lesions as a health indicator is an established practice and has been commonly used to monitor the health of pigs,” he observes. This has been confirmed by a number of studies.
“However, research delving into the possible association between carcass lesions and food-borne pathogen contamination at processing is lacking.”
This study highlights and quantifies the often-discussed one-health impact of veterinary care that “healthy pigs really do make safer food,” Hurd says.
The probability of salmonella contamination associated with carcass lesions observed in this study may seem like a small increase compared with epidemiological standards. “However, when applied to the 95 million pigs harvested annually in the United States, the implications for public health are nontrivial,” Hurd says. “For example, if the prevalence of carcasses with lesions increased by 50% (from 7.1% to 10.7%), that would add 140,220 salmonella-contaminated carcasses to the U.S. food supply.”
Sidebar
Animal Welfare Group Rebuts Stance on Antibiotic Resistance
Animal Welfare Approved, an Alexandria, VA-based animal welfare group, has called a recent paper discounting the link between farm antibiotic use and the development of antibiotic-resistant disease in humans as “misleading” and “highly irresponsible.”
Researchers at the United Kingdom’s University of Glasgow compared the development of antibiotic resistance in animals and people in Scotland for Salmonella typhimurium DT 104 — a bacterium that is considered a major source of food poisoning in humans.
Scottish researchers concluded that the local animal populations were “unlikely to be the major source of resistance diversity for humans.” As a result, the “current policy emphasis on restricting antimicrobial use in domestic animals may be overly simplistic,” they suggested.
A number of agricultural interests reacted by using that research to criticize attempts to impose restrictions on the use of antibiotics in farming. Their argument is that the paper suggests the use of antibiotics in animal agriculture is not a major contributor to the development of antibiotic resistance in diseases that affect humans.
But Animal Welfare Approved says the University of Glasgow researchers’ conclusions stand in contrast to over 50 years of research in this scientific endeavor and contradict the position of a number of notable national and international authorities.
Andrew Gunther, program director for Animal Welfare Approved, says the research presents some “highly perplexing” conclusions. “For example, why did they choose to effectively hide the fact that the antibiotic-resistant salmonella types that originated in humans only — and not as a result of the use of antibiotic use in farming — actually accounts for less than 2% of all human cases of the disease?
“And why did they fail to tell us whether the types of antibiotic-resistant salmonella that affect both humans and animals first originated in either humans or animals and, thus, establish whether or not factory farming is to blame?”
Gunther says, “This research paper should have been published with far more modest and balanced conclusions.”
About the Author(s)
You May Also Like





