Hog Health
thumbnail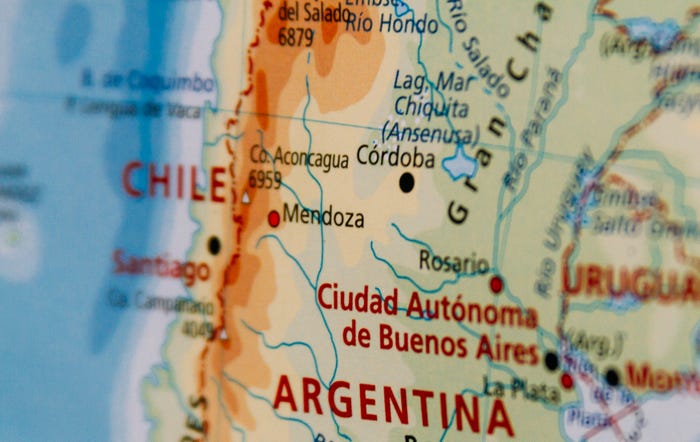
Livestock Management
Chile eradicates porcine reproductive and respiratory syndromeChile eradicates porcine reproductive and respiratory syndrome
PRRS costs the U.S. pork industry $664 million a year.
Subscribe to Our Newsletters
National Hog Farmer is the source for hog production, management and market news





.jpg?width=300&auto=webp&quality=80&disable=upscale)