For many years, pig heart valves have been used successfully for replacing valves in humans.
January 11, 2022
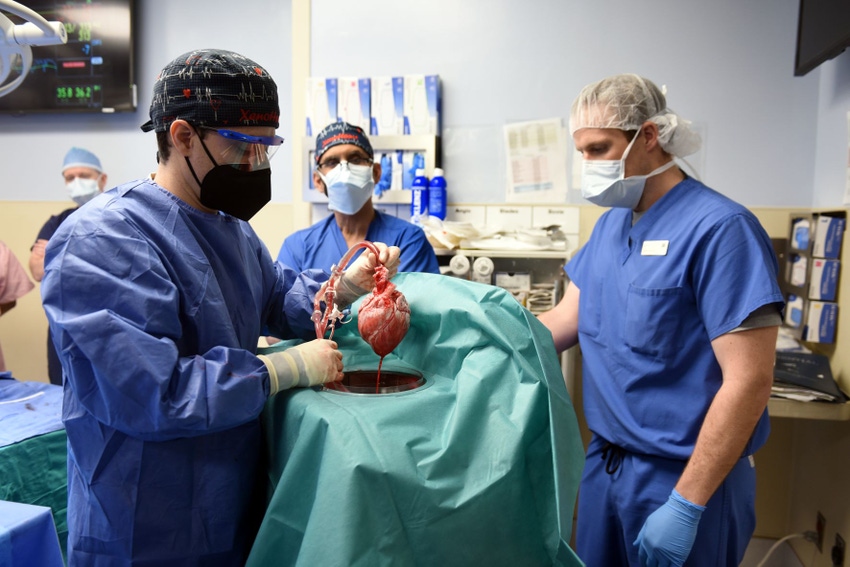
In a first-of-its-kind surgery, a 57-year-old patient with terminal heart disease received a successful transplant of a genetically-modified pig heart and is still doing well three days later. It was the only currently available option for the patient. The historic surgery was conducted by University of Maryland School of Medicine (UMSOM) faculty at the University of Maryland Medical Center (UMMC), together known as the University of Maryland Medicine.
This organ transplant demonstrated for the first time that a genetically-modified animal heart can function like a human heart without immediate rejection by the body. The patient, David Bennett, a Maryland resident, is being carefully monitored over the next days and weeks to determine whether the transplant provides lifesaving benefits. He had been deemed ineligible for a conventional heart transplant at UMMC as well as at several other leading transplant centers that reviewed his medical records.
"It was either die or do this transplant. I want to live. I know it's a shot in the dark, but it's my last choice," said Bennett, a day before the surgery was conducted. He had been hospitalized and bedridden for the past few months. "I look forward to getting out of bed after I recover."
The U.S. Food and Drug Administration granted emergency authorization for the surgery on New Year's Eve through its expanded access (compassionate use) provision. It is used when an experimental medical product, in this case the genetically-modified pig's heart, is the only option available for a patient faced with a serious or life-threatening medical condition. The authorization to proceed was granted in the hope of saving the patient's life.
"This was a breakthrough surgery and brings us one step closer to solving the organ shortage crisis. There are simply not enough donor human hearts available to meet the long list of potential recipients," said Bartley P. Griffith, MD, who surgically transplanted the pig heart into the patient. Dr. Griffith is the Thomas E. and Alice Marie Hales distinguished professor in Transplant Surgery at UMSOM and director of the Cardiac Transplant Program at UMMC. "We are proceeding cautiously, but we are also optimistic that this first-in-the-world surgery will provide an important new option for patients in the future."
Considered one of the world's foremost experts on transplanting animal organs, known as xenotransplantation, Muhammad M. Mohiuddin, MD, professor of Surgery at UMSOM, joined the UMSOM faculty five years ago and established the Cardiac Xenotransplantation Program with Dr. Griffith. Dr. Mohiuddin serves as the program's scientific/program director and Dr. Griffith as its clinical director.
"This is the culmination of years of highly complicated research to hone this technique in animals with survival times that have reached beyond nine months. The FDA used our data and data on the experimental pig to authorize the transplant in an end-stage heart disease patient who had no other treatment options," said Dr. Mohiuddin. "The successful procedure provided valuable information to help the medical community improve this potentially life-saving method in future patients."
About 110,000 Americans are currently waiting for an organ transplant, and more than 6,000 patients die each year before getting one, according to the federal government's Organ Donor page. Xenotransplantation could potentially save thousands of lives but does carry a unique set of risks, including the possibility of triggering a dangerous immune response. These responses can trigger an immediate rejection of the organ with a potentially deadly outcome to the patient.
Xenotransplants were first tried in the 1980s, but were largely abandoned after the famous case of Stephanie Fae Beauclair (known as Baby Fae) at Loma Linda University in California. The infant, born with a fatal heart condition, received a baboon heart transplant and died within a month of the procedure due to the immune system's rejection of the foreign heart. However, for many years, pig heart valves have been used successfully for replacing valves in humans.
Before consenting to receive the transplant, Mr. Bennett, the patient, was fully informed of the procedure's risks, and that the procedure was experimental with unknown risks and benefits. He had been admitted to the hospital more than six weeks earlier with life-threatening arrythmia and was connected to a heart-lung bypass machine, called extracorporeal membrane oxygenation (ECMO), to remain alive. In addition to not qualifying to be on the transplant list, he was also deemed ineligible for an artificial heart pump due to his arrhythmia.
Revivicor, a regenerative medicine company based in Blacksburg, Virginia, provided the genetically-modified pig to the xenotransplantation laboratory at UMSOM. On the morning of the transplant surgery, the surgical team, led by Dr. Griffith and Dr. Mohiuddin, removed the pig's heart and placed it in the XVIVO Heart Box, perfusion device, a machine that keeps the heart preserved until surgery.
Organs from genetically modified pigs have been the focus of much of the research in xenotransplantation, in part because of physiologic similarities between pigs, human, and nonhuman primates. UMSOM received $15.7 million sponsored research grant to evaluate Revivicor genetically-modified pig UHearts in baboon studies.
Three genes—responsible for rapid antibody-mediated rejection of pig organs by humans—were "knocked out" in the donor pig. Six human genes responsible for immune acceptance of the pig heart were inserted into the genome. Lastly, one additional gene in the pig was knocked out to prevent excessive growth of the pig heart tissue, which totaled 10 unique gene edits made in the donor pig.
Dr. Mohiuddin, Dr. Griffith and their research team spent the past five years perfecting the surgical technique for transplantation of pig hearts into non-human primates. Dr. Mohiuddin's xenotransplant research experience spans over 30 years during which time he demonstrated in peer-reviewed research that genetically-modified pig's hearts can function when placed in the abdomen for as long as three years. Success was dependent on the right combination of genetic modifications to the experimental donor pig UHeart and anti-rejection drugs, including some experimental compounds.
You May Also Like



